For this article, journalist Judith Graham interviewed doctors about how time-consuming and difficult it can be for older patients to get the health care they need. When you add up the time they spend on everything from medical tests and doctor visits to juggling appointments and dealing with insurance companies, it comes to about three weeks a year for most. Graham has some suggestions for how to lighten that burden. KFF Health News posted her article on March 27, 2024. It also ran on the Washington Post. Funding from the Silver Century Foundation helps KFF Health News develop articles (like this one) on longevity and related health and social issues.
Susanne Gilliam, 67, was walking down her driveway to get the mail in January when she slipped and fell on a patch of black ice.
Pain shot through her left knee and ankle. After summoning her husband on her phone, with difficulty she made it back to the house.
And then began the run-around that so many people face when they interact with America’s uncoordinated health care system.
Gilliam’s orthopedic surgeon, who managed previous difficulties with her left knee, saw her that afternoon but told her, “I don’t do ankles.”
He referred her to an ankle specialist who ordered a new set of X-rays and an MRI. For convenience’s sake, Gilliam asked to get the scans at a hospital near her home in Sudbury, MA. But the hospital didn’t have the doctor’s order when she called for an appointment. It came through only after several more calls.
Coordinating the care she needs to recover, including physical therapy, became a part-time job for Gilliam. (Therapists work on only one body part per session, so she has needed separate visits for her knee and for her ankle several times a week.)
“The burden of arranging everything I need—it’s huge,” Gilliam told me. “It leaves you with such a sense of mental and physical exhaustion.”
The toll the American health care system extracts is, in some respects, the price of extraordinary progress in medicine. But it’s also evidence of the poor fit between older adults’ capacities and the health care system’s demands.
“The good news is we know so much more and can do so much more for people with various conditions,” said Thomas H. Lee, MD, chief medical officer at Press Ganey, a consulting firm that tracks patients’ experiences with health care. “The bad news is the system has gotten overwhelmingly complex.”
We don’t talk enough about what we’re asking older adults to do and whether that’s realistic.
— Ishani Ganguli, MD
That complexity is compounded by the proliferation of guidelines for separate medical conditions, financial incentives that reward more medical care, and specialization among clinicians, said Ishani Ganguli, MD, an associate professor of medicine at Harvard Medical School.
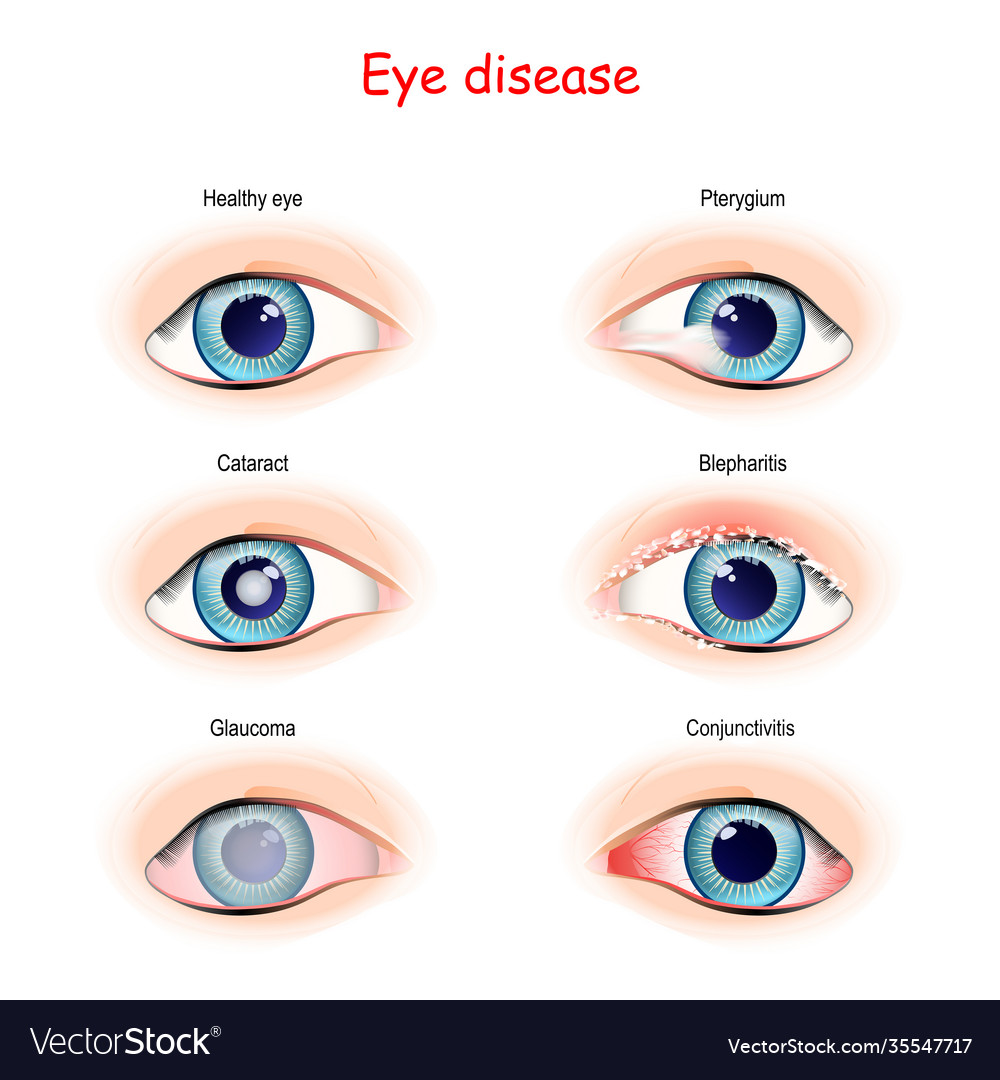
“It’s not uncommon for older patients to have three or more heart specialists who schedule regular appointments and tests,” she said. If someone has multiple medical problems—say, heart disease, diabetes, and glaucoma—interactions with the health care system multiply.
Ganguli is the author of a new study showing that Medicare patients spend about three weeks a year having medical tests, visiting doctors, undergoing treatments or medical procedures, seeking care in emergency rooms or spending time in the hospital or rehabilitation facilities. (The data is from 2019, before the COVID pandemic disrupted care patterns. If any services were received, that counted as a day of health care contact.)
That study found that slightly more than 1 in 10 seniors, including those recovering from or managing serious illnesses, spent a much larger portion of their lives getting care—at least 50 days a year.
“Some of this may be very beneficial and valuable for people, and some of it may be less essential,” Ganguli said. “We don’t talk enough about what we’re asking older adults to do and whether that’s realistic.”
Victor Montori, MD, a professor of medicine at the Mayo Clinic in Rochester, MN, has for many years raised an alarm about the “treatment burden” that patients experience. In addition to time spent receiving health care, this burden includes arranging appointments, finding transportation to medical visits, getting and taking medications, communicating with insurance companies, paying medical bills, monitoring health at home and following recommendations such as dietary changes.
More and more medical practices use online patient portals and digital phone systems that frustrate older patients, who find them hard to navigate.
Four years ago—in a paper titled “Is My Patient Overwhelmed?”—Montori and several colleagues found that 40 percent of patients with chronic conditions such as asthma, diabetes and neurological disorders “considered their treatment burden unsustainable.”
When this happens, people stop following medical advice and report having a poorer quality of life, the researchers found. Especially vulnerable are older adults with multiple medical conditions and low levels of education who are economically insecure and socially isolated.
Older patients’ difficulties are compounded by medical practices’ increased use of digital phone systems and electronic patient portals—both frustrating for many seniors to navigate—and the time pressures afflicting physicians. “It’s harder and harder for patients to gain access to clinicians who can problem-solve with them and answer questions,” Montori said.
Meanwhile, clinicians rarely ask patients about their capacity to perform the work they’re being asked to do. “We often have little sense of the complexity of our patients’ lives and even less insight into how the treatments we provide (to reach goal-directed guidelines) fit within the web of our patients’ daily experiences,” several physicians wrote in a 2022 paper on reducing treatment burden.
Consider what Jean Hartnett, 53, of Omaha, NE, and her eight siblings went through after their 88-year-old mother had a stroke in February 2021 while shopping at Walmart.
At the time, the older woman was looking after Hartnett’s father, who had kidney disease and needed help with daily activities such as showering and going to the bathroom.
During the year after the stroke, both of Hartnett’s parents—fiercely independent farmers who lived in Hubbard, NE,—suffered setbacks, and medical crises became common. When a physician changed her mom’s or dad’s plan of care, new medications, supplies and medical equipment had to be procured, and new rounds of occupational, physical and speech therapy arranged.
Neither parent could be left alone if the other needed medical attention.
“It wasn’t unusual for me to be bringing one parent home from the hospital or doctor’s visit and passing the ambulance or a family member on the highway taking the other one in,” Hartnett explained. “An incredible amount of coordination needed to happen.”
Hartnett moved in with her parents during the last six weeks of her father’s life, after doctors decided he was too weak to undertake dialysis. He passed away in March 2022. Her mother died months later in July.
Ask which of the things you’re being asked to do is most important and which might be expendable.
So, what can older adults and family caregivers do to ease the burdens of health care?
To start, be candid with your doctor if you think a treatment plan isn’t feasible and explain why you feel that way, said Elizabeth Rogers, MD, an assistant professor of internal medicine at the University of Minnesota Medical School.
“Be sure to discuss your health priorities and trade-offs: what you might gain and what you might lose by forgoing certain tests or treatments,” she said. Ask which interventions are most important in terms of keeping you healthy, and which might be expendable.
Doctors can adjust your treatment plan, discontinue medications that aren’t yielding significant benefits and arrange virtual visits if you can manage the technological requirements. (Many older adults can’t.)
Ask if a social worker or a patient navigator can help you arrange multiple appointments and tests on the same day to minimize the burden of going to and from medical centers. These professionals can also help you connect with community resources, such as transportation services, that might be of help. (Most medical centers have staff of this kind, but physician practices do not.)
If you don’t understand how to do what your doctor wants you to do, ask questions: What will this involve on my part? How much time will this take? What kind of resources will I need to do this? And ask for written materials, such as self-management plans for asthma or diabetes, that can help you understand what’s expected.
“I would ask a clinician, ‘If I chose this treatment option, what does that mean not only for my cancer or heart disease but also for the time I’ll spend getting care?’” said Ganguli of Harvard. “If they don’t have an answer, ask if they can come up with an estimate.”

Judith Graham writes a column on aging and health for KFF Health News, where she’s a contributing columnist. She also freelances for other publications. Earlier in her career, Judith contributed more than 80 pieces to the New York Times blog, The New Old Age. She was nominated for a Pulitzer Prize for a series on defective pacemakers and was part of a Chicago Tribune team that won a Pulitzer in 2001.