What kind of hospital care would you want if you had COVID-19 and were desperately ill? In this article, journalist Judith Graham pulls together the facts about treatments, especially with ventilators, along with expert advice on what to do and how to decide. Her article was posted on the KHN website on May 12, 2020, and also ran on the Washington Post.
DENVER ― Last month, Minna Buck revised a document specifying her wishes should she become critically ill.
“No intubation,” she wrote in large letters on the form, making sure to include the date and her initials.
Buck, 91, had been following the news about COVID-19. She knew her chances of surviving a serious bout of the illness were slim. And she wanted to make sure she wouldn’t be put on a ventilator under any circumstances.
“I don’t want to put everybody through the anguish,” said Buck, who lives in a continuing care retirement community in Denver.
For older adults contemplating what might happen to them during this pandemic, ventilators are a fraught symbol, representing a terrifying lack of personal control as well as the fearsome power of technology.
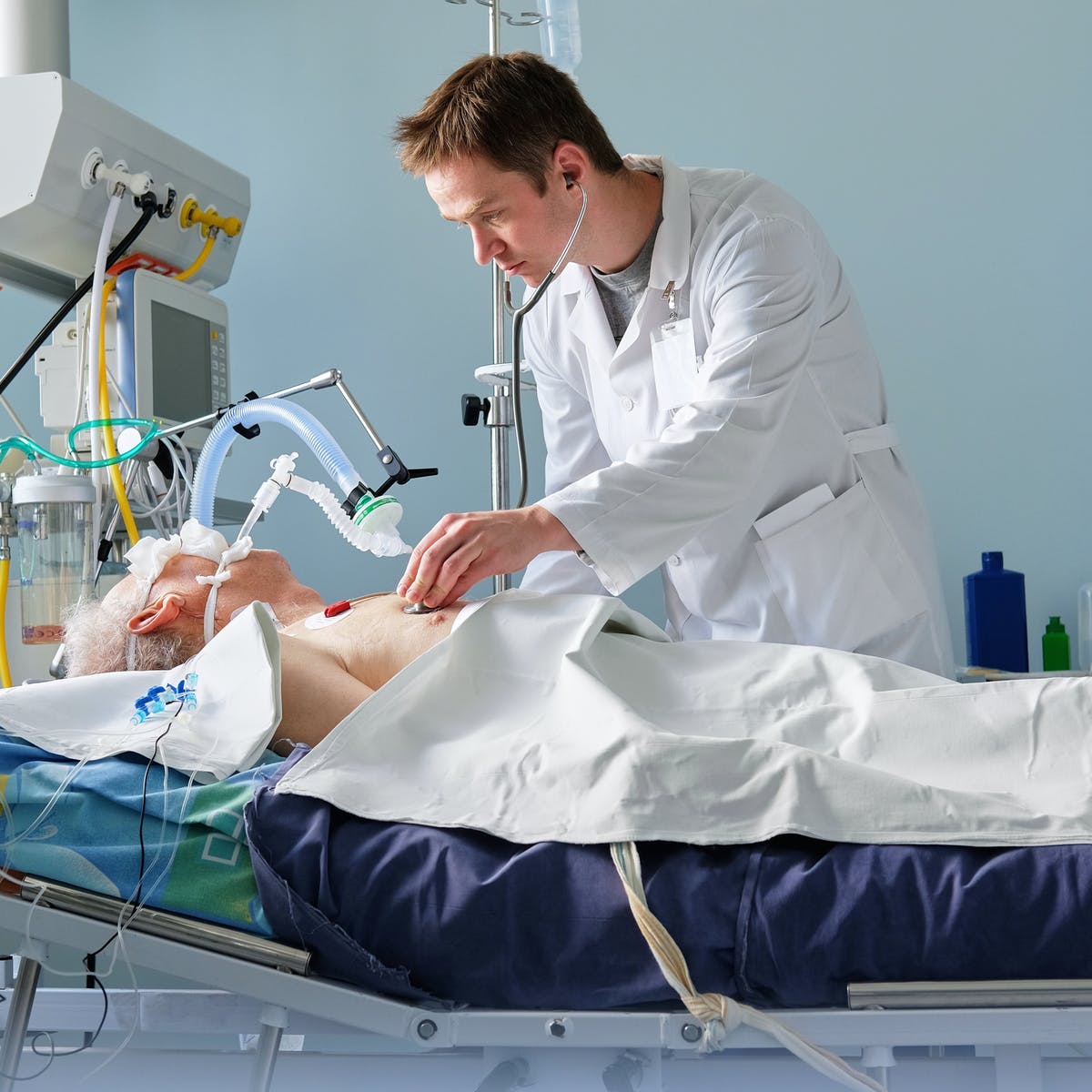
Used for people with respiratory failure, a signature consequence of severe COVID-19, these machines pump oxygen into a patient’s body while he or she lies in bed, typically sedated, with a breathing tube snaked down the windpipe (known as “intubation”).
For some seniors, this is their greatest fear: being hooked to a machine, helpless, with the end of life looming. For others, there is hope that the machine might pull them back from the brink, giving them another shot at life.
“I’m a very vital person: I’m very active and busy,” said Cecile Cohan, 85, who has no diagnosed medical conditions and lives independently in a house in Denver. If she became critically ill with COVID-19 but had the chance of recovering and being active again, she said, “yes, I would try a ventilator.”
Out of all those who become infected with COVID-19, frail older adults are the least likely to survive treatment with a ventilator.
What’s known about people’s chances?
Although several reports have come out of China, Italy and, most recently, the area around New York City, “the data is really scanty,” said Carolyn Calfee, a professor of anesthesia at the University of California-San Francisco [UCSF].
Initial reports suggested that the survival rate for patients on respirators ranged from 14 percent (Wuhan, China) to 34 percent (early data from the United Kingdom). A report from the New York City Area appeared more discouraging, with survival listed at only 11.9 percent.
But the New York data incorporated only patients who died or were discharged from hospitals—a minority of a larger sample. Most ventilator patients were still in the hospital, receiving treatment, making it impossible for researchers to draw reliable conclusions.
Calfee worries that data from these early studies may not apply to US patients treated in hospitals with considerable resources.
“The information we have is largely from settings with tremendous resource gaps and from hospitals that are overwhelmed, where patients may not be treated with optimal ventilator support,” she said. “I would be very worried if people used that data to make decisions about whether they wanted mechanical ventilation.”
Still, a sobering reality emerges from studies published to date: older adults, especially those with underlying medical conditions such as heart, kidney or lung disease, are least likely to survive critical illness caused by the coronavirus or treatment with a ventilator.
“Their prognosis is not great,” said Douglas White, MD, a professor of critical care medicine at the University of Pittsburgh. He cautioned, however, that frail older adults shouldn’t be lumped together with healthy, robust older adults, whose prospects may be somewhat better.
The choice isn’t as black-and-white as go on a ventilator or die.
Like other clinicians, White has observed that older COVID patients are spending considerably longer on ventilators—two weeks or more—than is the case with other critical illnesses. If they survive, they’re likely to be extremely weak, deconditioned, suffering from delirium and in need of months of ongoing care and physical rehabilitation.
“It’s a very long, uphill battle to recovery,” and many older patients may never regain full functioning, said Negin Hajizadeh, MD, an associate professor of critical care medicine at the School of Medicine at Hofstra/Northwell on New York’s Long Island. “My concern is, who’s going to take care of these patients after a prolonged ventilator course—and where?”
In St. Paul, MN, Joyce Edwards, 61, who is unmarried and lives on her own, has been wondering the same thing.
In late April, Edwards revised her advance directive to specify that “for COVID-19, I do not want to be placed on a ventilator.” Previously, she had indicated that she was willing to try a ventilator for a few days but wanted it withdrawn if the treatment was needed for a longer period.
“I have to think about what the quality of my life is going to be,” Edwards said. “Could I live independently and take care of myself—the things I value the most? There’s no spouse to take care of me or adult children. Who would step into the breach and look after me while I’m in recovery?”
People who’ve said “give a ventilator a try but discontinue it if improvement isn’t occurring” need to realize that they almost surely won’t have time to interact with loved ones if treatment is withdrawn, said Christopher Cox, MD, an associate professor of medicine at Duke University.
“You may not be able to live for more than a few minutes,” he noted.
But the choice isn’t as black-and-white as go on a ventilator or die.
“We can give you high-flow oxygen and antibiotics,” Cox said. “You can use BiPAP or CPAP machines [which also deliver oxygen] and see how those work. And if things go poorly, we’re excellent at keeping you comfortable and trying to make it possible for you to interact with family and friends instead of being knocked out in a coma.”
People are thinking about what could happen to them and they want to talk about it. It’s opened up a lot of conversations.
— Rebecca Sudore, MD
Heather McCrone of Bellevue, WA, realized she’d had an “all-or-nothing” view of ventilation when her 70-year-old husband developed sepsis—a systemic infection—last year after problems related to foot surgery.
Over nine hours, McCrone sat in the intensive care unit as her husband was stabilized on a ventilator by nurses and respiratory therapists. “They were absolutely fantastic,” McCrone said. After a four-day stay in the hospital, her husband returned home.
“Before that experience, my feeling about ventilators was, ‘You’re a goner and there’s no coming back,’” McCrone said. “Now, I know that’s not necessarily the case.”
She and her husband both have advance directives stating that they want “lifesaving measures taken unless we’re in a vegetative state with no possibility of recovery.” McCrone said they still need to discuss their wishes with their daughters, including their preference for getting treatment with a ventilator.
These discussions are more important than ever―and perhaps easier than in the past, experts said.
“People are thinking about what could happen to them and they want to talk about it,” said Rebecca Sudore, MD, a professor of medicine at the UCSF. “It’s opened up a lot of conversations.”
Rather than focusing on whether to be treated with a ventilator, she advises older adults to discuss what’s most important to them—independence? time with family? walking? living as long as possible?—and what they consider a good quality of life. This will provide essential context for decisions about ventilation.
“Some people may say, my life is always worth living no matter what type of serious illness or disability I have,” she said. “On the other end of the spectrum, some people may feel there are health situations or experiences that would be so hard that life would not be worth living.”
Sudore helped create Prepare for Your Care, a website and a set of tools to guide people through these kinds of conversations. Recently it was updated to include a section on COVID-19, as have sites sponsored by Compassion & Choices and The Conversation Project. And the Colorado Program for Patient Centered Decisions has published a decision aid for COVID patients considering life support, also available in Spanish.
Some older adults have another worry: What if there aren’t enough ventilators for all the COVID patients who need them?
In that situation, “I would like to say ‘no’ because other people need that intervention more than I do and would benefit, in all probability, more than I would,” said Larry Churchill, 74, an emeritus professor of medical ethics at Vanderbilt.
“In a non-scarcity situation, I’m not sure what I’d do. I’m in pretty good health, but people my age don’t survive as well from any major problem,” Churchill said. “Most of us don’t want a long, lingering death in a custodial facility where the chances of recovery are small and the quality of life may be one we’re not willing to tolerate.”

Judith Graham writes a column on aging and health for KFF Health News, where she’s a contributing columnist. She also freelances for other publications. Earlier in her career, Judith contributed more than 80 pieces to the New York Times blog, The New Old Age. She was nominated for a Pulitzer Prize for a series on defective pacemakers and was part of a Chicago Tribune team that won a Pulitzer in 2001.